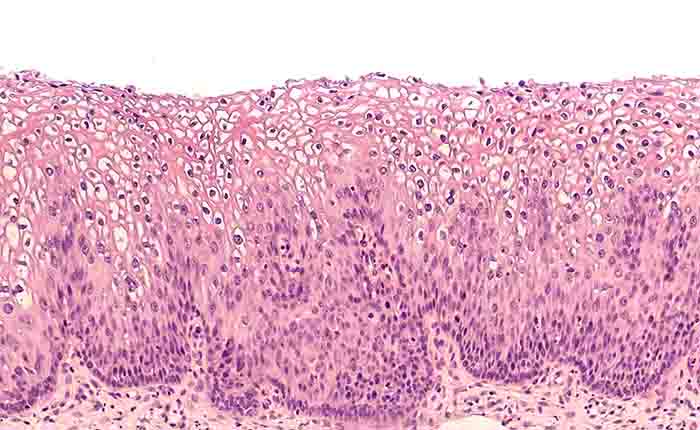
Cervical Abnormalities
What are cervical abnormalities caused by?
The vast majority of cervical abnormalities are the result of long-term, persistent HPV infection. HPV is a rather common infection. According to literature, at least 80% of women will be infected with one or more subtypes of the virus soon after they commence their sexual life. In most cases, the immune system will successfully control the infection by suppressing it within 2 years.
Cervical abnormalities: What happens when HPV infection remains active?
If the infection remains active, a number of women will develop persistent infection which, however, fails to cause cervical lesions.
Some women with persistent HPV infection develop low-grade intraepithelial lesion (Low Grade Squamous Intraepithelial Lesion – LGSIL or Cervical Intraepithelial Neoplasia grade 1 – CIN1). The majority of low-grade lesions regresses automatically (70-90%). Amongst the remaining, some will remain at this stage for years and the rest will progress to high-grade lesions (High Grade Squamous Intraepithelial Lesion – HGSIL or Cervical Intraepithelial Neoplasia grade 2-3 – CIN2-3).
Finally, some of the women with neglected high-grade lesions will develop invasive cervical cancer if left untreated for years.
Cervical abnormalities: Conservative management
HPV infection as well as low-grade cervical lesions are usually managed with simple monitoring. The individual decision for each woman depends on:
• her age
• her medical history
• the presence of risk factors
• the desire for future pregnancies
• Her preference and the informed decision she will make following a detailed consultation of the pros and cons of each approach by an expert gynaecologist
Smoking cessation is known to double the success rate of HPV suppression by the immune system. The use of condom has also been found to have a positive effect to clearing HPV infection and hence controlling cervical lesions. Also, some commercially available medical treatments, that aim to boost the immune response against HPV, can have a positive contribution.
The treatments listed below do not alter the long term risk of HPV infection. They are however likely to help clear it shortly after treatment by reducing the viral load and initiating an immune response. Interestingly, the likelihood of persistent infection and/or re-infection following treatment for persistent low-grade lesions is very high, and higher compared to if the treatment is performed for a high-grade abnormality.
Cervical abnormalities: Invasive treatments
Excisional treatments for cervical lesions (loop excision, LLETZ, LEEP, cone biopsy, cold knife conisation) are the indicated treatment for:
• some of the moderate changes (CIN2)
• Severe changes (CIN3)
Excisional treatments aim to remove the area around the opening of the cervix where the abnormalities occur. Treatments can be performed both under local and general anesthetic as a day case and are extremely safe. Provided they are properly performed by a trained gynaecologist, the risk of complications, both short and long term, is very low. In addition, they are very successful in removing the lesion and normalise cytology in >95% of cases.
Increasing data in the literature show that vaccination after treatment for high-grade cervical intraepithelial lesions increases protection against re-infection. Therefore, vaccination after treatment reduces the risk of future recurrence of the lesion. This appears to be due to the high probability of short-term suppression of HPV infection immediately after excisional treatment for high-grade abnormalities.
Who can I turn to for cervical abnormalities?
Gynaecologist Surgeon Christina Founta has extensive experience in diagnosis, management and treatment of HPV related cervical abnormalities. She is accredited in Diagnostic Colposcopy and Treatment, as well as a trainer of the British Society of Cervical Colposcopy and Pathology (BSCCP) for a number of years. She is also one of the few private gynecologists in Greece certified in therapeutic colposcopy by the Hellenic Society of Colposcopy and Cervical Pathology.